- Future Students
- Current Students
- Faculty
- Staff
- Alumni
- Others
Words and Pictures by Corbin Smith
Where are they now?
Corbin Smith (Media Studies ’10)

The idea for this story came to Corbin Smith while playing hockey.
A teammate of his works as a paramedic. “He would say, People just don’t realize what our job entails. That made me think.”
And so he pitched the idea to The Grid, a Toronto weekly.
“I thought showing the difference between the public perception of a paramedic and their reality would be great. A photo essay, showing a day in the life of a Toronto EMS worker.”
He continues: “My general interest is to learn new things. That’s what gets me excited. And part of the excitement of storytelling is that you get to share stories and make others excited.”
“It’s great that I get to do this as a job.”
Since graduating from the University of Guelph-Humber in 2010, Smith's photographs have been published in Torontoist, Now Magazine, The Grid, The Toronto Star, The Globe and Mail, National Post, Lush Magazine, and Library Journal Magazine.
Lately, though, he’s found himself writing the stories to go with his pictures.
“Anyone can take a photo now with a smartphone or a decent camera; I set myself apart by telling distinct and interesting stories. And you need more than a camera to be able to do that.”
Smith talks of the changing landscape of journalism and publishing: “Who knows what will happen. But I can – and have - transferred my skills from photojournalism to art photography to commercial and advertising to documentary. I'm now recognized as someone who can shoot and write.”
“It’s not easy and it’s not glamorous – any photographer would tell you that. But I get to be an explorer of people, art and culture in my own town. It’s pretty cool.”
See and read Corbin Smith’s story, What is it like to work a 12-hour EMS shift?
Published in The Grid.
If you’re lucky, you’ve never had to meet an Emergency Medical Services Paramedic (and we mean that in the nicest way possible). We followed a couple of teams on two different shifts to see what they experience on a typical day.
BY: CORBIN SMITH
Day One
Who: Paul Roberts, PCP, and Drew Crocker, PCP (Primary Care Paramedics). Crocker was on his last day of a six-month training period and went full-time at midnight, a few hours before the end of the shift.
1. TTC driver call
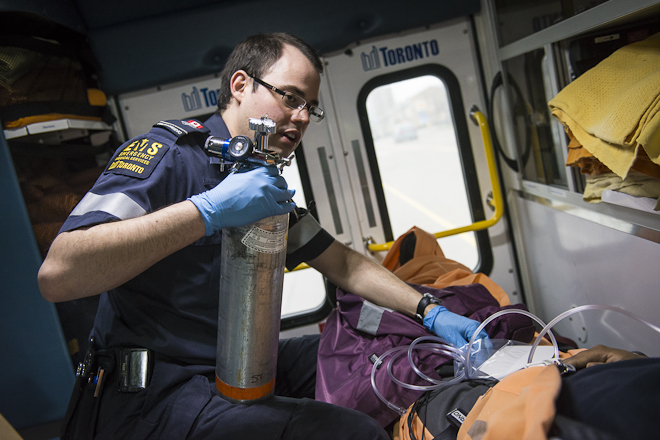
Roberts and Crocker had to administer oxygen to a TTC operator who suddenly felt ill during his bus route. The patient was also complaining of tingling and numbness, so there was some concern about his heart. “Based on the information we have, we treat for the worst-case scenario but always hope for the best,” said Roberts (pictured).

2. Typical call
More often than not, calls are a moderate urgency level—a CTAS3 on the Canadian Triage and Acuity Scale. Roberts suggests that, on average, he sees the highest emergency level (CTAS1) only about once a week. The team’s second patient of the day was a hockey player who sustained a shoulder injury after being checked into the boards. The patient was in so much pain, however, that his face began to go numb, so the only way to remove his gear and get him on the stretcher was to cut through his equipment.

3. The nature of EMS shift work
In their penultimate call of the day, Crocker and Roberts responded to a situation in which an older woman was experiencing some shortness of breath. The call went quickly: It came in at 10:20 p.m. and wrapped up when they transferred the patient to the hospital at 11:23 p.m. Although they were nearing the end of their shift “working the twos” (2 p.m. to 2 a.m.), Crocker and Roberts didn’t actually finish their day until closer to 4 a.m.

4. Different kinds of paramedics
While all paramedics go though the same basic training, there are many different EMS specializations in Toronto. Most people have heard of Primary Care Paramedics and Advanced Care Paramedics (ACP), who operate out of the ambulances we see on city streets. Less familiar are the paramedics who are part of units such as the Toronto Emergency Task Force, Heavy Urban Search and Rescue, the marine unit, and the bicycle unit.
Day Two
Who: Jonathan Mak, PCP, and Scarlett Martyn, ACP.

5. Unique equipment
Mak and Martyn assisted an elderly woman into a specialty stretcher, which allows paramedics to safely transport patients up and down stairs.

6. Offload delay
Paramedics must remain with their patient in the hospital until care has been transferred to a registered nurse—what’s referred to as “offload delay.” Unless a patient needs immediate lifesaving intervention, paramedics expect some degree of offload delay with every call. (Roberts says that with no delay, they’d be in and out of the hospital in about 45 minutes.) “The longest offload-delay I ever experienced was 11.5 hours,” he said, “but that was an incredibly rare situation. In the early 2000s, offload delay times were really bad, and while it has gotten much better since then, I’d say the average is anywhere from one to two hours.”

7. Non-medical duties
While downtime is rare, paramedics are expected to keep on top of the more mundane duties, like keeping their truck clean inside and out and making sure there’s enough gas in the tank.

8. EMS and other emergency workers
Minutes before their 12-hour shift was over, Mak and Martyn were called to respond to what turned out to be an inebriated man passed out at Jane and Finch. When their patient regained consciousness en route to the hospital, there was a short violent outburst. Mak easily avoided the attack, reprimanded the patient for his behaviour, and then carried on with his diagnostic tests and patient care. “It’s pretty rare that anything like that happens,” said Mak, once the situation calmed down. “In situations where there is a medical emergency and the threat of violence, both EMS and the police will be called to the scene. We’re not equipped to do their job and the police can’t do what we do—we work together.”

EMS STATS
65: Number of paramedics the city plans to hire by the end of this year.
850: Number of paramedics on staff right now.
155: Number of vehicles in Toronto’s EMS fleet.
182,000: Average number of patients transported by Toronto EMS each year.
500: Average number of patients transported each day.
200: Number of 911 calls David Lee Roth responded to during his post–Van Halen career as an EMT worker in New York City.

